Many couples face the problem of conception. 40 years ago, back in 1978, the first person conceived through IVF was born in Britain – a girl named Louise Brown. This revolutionary method brought happiness to many childless couples, and the creator of the IVF method, Robert Edwards, received the Nobel prize.
When should a couple who is having trouble conceiving raise the alarm?
If attempts to conceive naturally within a year do not give results, it is worth turning to a reproductologist. It is important not to waste time, because the ovarian reserve of a woman worsens with age, and therefore the chances of a favorable outcome decrease! In addition, gynecologists now have many options for solving infertility problems, including IVF.
What is the essence of this procedure?
IVF literally stands for in vitro fertilization. Its basic formula: artificially stimulate the growth of several follicles in the ovaries, when they reach the ovulatory size, safely extract them from the body, fertilize them in a special environment, wait a few days to realize that the embryo began to develop, and introduce this embryo into the uterine cavity. In fact, this is exactly what fertility doctors do, together with embryologists, who carry out the sacrament of fertilization.
It would seem that everything is simple, you combine an egg with a sperm cell, put it in the uterus – and that’s the pregnancy?
Unfortunately, this is not always the case. The efficiency of IVF varies greatly from 20 to 70%, because it depends on the problem which IVF solves. Actually with the advent of this technology it became clear that not everything is clear in reproductive matters, and what seemed clear is not. In fact, no reproductologist can say with certainty that a pregnancy will occur after the insertion of a developing embryo into the uterine cavity, even if he is absolutely certain that everything was done well and correctly. We are a long way from fully understanding the pregnancy process, but we can already help a growing number of previously childless couples.
What is the best way to prepare for your first reproductive visit?
If a woman realizes that she cannot get pregnant without assisted reproductive technology, she should choose a clinic and go for her first visit. You should plan your visit to a reproductologist during the first days after menstruation, although this is not a matter of principle, as the information content of the menstrual cycle depends on the gynecological problem. For example, the reason for infertility is generally clear – the tubal factor, no other changes – a visit at the beginning of the cycle, in this case the doctor will focus on the ovarian reserve. Another situation – there was uterine inflammation after the abortion or you tried to stop the bleeding by curettage, after that menstruation became scarce – then plan your visit better in the second phase of the cycle or in the middle – the doctor will estimate the maximum thickness of the endometrium and the consultation will be much more informative.
What tests should be done in advance and taken with you?
In order to benefit as much as possible from the first visit to the doctor and to reduce the number of follow-up visits, it is worth taking the previous examinations and tests with you and putting them in chronological order, so the doctor does not waste time on “working with the archive”. In addition, it is important to prepare a menstrual calendar (to clarify when the last menstruation took place; separately write out the duration of cycles, if they were not regular). It will also be necessary to remember in advance what diseases you have had in your entire life, what surgeries you have had, and whether you are currently taking any medications.
In addition to the tips listed above, at your first visit to the reproductologist you should bring some fresh tests:
– Spermogram – it’s important to have it done at the clinic you and your husband are going to. Since it takes four days to prepare for this examination, your husband or partner should be sent to the clinic in advance so that the results are ready for your visit. Spermogram is necessary to make a decision on the presence or absence of male infertility factor, and if it is present – the decision of the issue of IVF option selection.
– Blood tests for FSH, LH, estradiol, testosterone, AMH, inhibin, TTG and T4 free on day 2-3 of the cycle. Based on these tests, the doctor will be able to learn a lot and, in particular, assess the ovarian reserve of a woman, which affects the effectiveness of IVF with eggs, without the use of donor programs. Let me remind you, if according to ultrasound data at the beginning of the cycle a woman has very few follicles in the ovaries (3-5 in total), FSH exceeds 10-12 units, estradiol is reduced, and AMH less than one – ovarian reserve is considered low, and the effectiveness of ovulation stimulation is predicted as low.
– Cervical cytology smear. Performed by all women over the age of 21 to detect early cervical cell changes that could go the way of malignant transformation caused by the human papilloma virus. If a year has passed and you do not have a fresh smear – it is mandatory, because if it detects signs of initial cell changes (dysplasia), the treatment of infertility will need to be postponed and focus on cervical pathology. Of course, in preparation for IVF, additional tests are also appointed, some of them are routine, others will be determined by the specific situation, but these three points are important for the initial consultation.
And what happens next?
By the second visit, usually all the additional tests and examinations will be ready, on the basis of which the doctor can make his decision – is it necessary to make a correction of the identified changes that can improve the prognosis of pregnancy, or you can directly proceed to IVF. IVF program consists of several stages: stimulation of superovulation, egg collection, fertilization and obtaining embryos, cryopreservation of embryos and after, transferring embryos into the uterine cavity. Each stage has its own nuances.
In addition to classic IVF, there is often talk about ICSI. What is it?
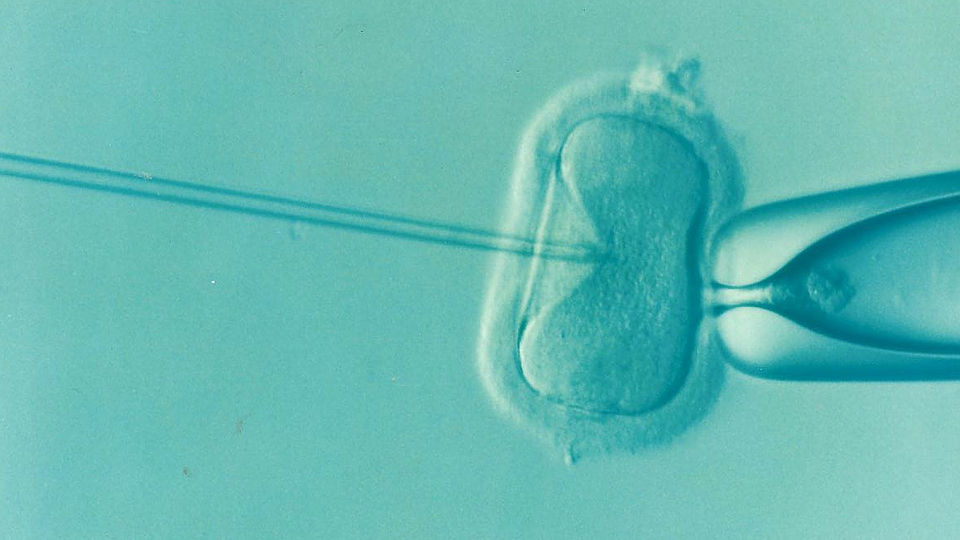
ICSI is not a Russian abbreviation, but simply the Russian sounding of the English (Intracytoplasmic sperm injection (ICSI)). The essence of the method is that only one (the best from the embryologist’s point of view) sperm is selected for fertilization, and it is injected into the egg manually. This method is used in cases where there is a poor quality of sperm, there are very few of them or there are problems with the shell of the egg, which is very difficult to destroy
A quite logical question arises – why not perform ICSI in all cases? With classical IVF we allow factors that are not fully known to us to select the sperm that will penetrate the egg. This approach preserves the naturalness of conception, we only create the conditions for an encounter that was not present in the infertile couple, for example due to an obstruction of the fallopian tubes. During ICSI, the selection of sperm is performed by a person specially trained, using knowledge and experience, which allows us to select the most “correct” sperm by external (important: only external) signs and introduce it into an oocyte. Let me remind you that the process of introducing a sperm is done manually, using a special microscope. In this case the embryologist’s hands become an additional artificial factor. It turns out that ICSI, as opposed to classic IVF, has a lot of artificial things, depending on the personality of the embryologist. You can read more about all of this, as well as the various nuances of IVF, in my book “A Good Book for the Future Mama” (Eksmo Publishing House).
– In 1982, Louise Brown’s first “test-tube baby” had a sister, Natalie, also conceived through IVF. In our country, the first baby born through IVF was a girl named Lena, who was born in 1986.
– There is a common belief that people born through IVF are infertile. They are not! The same sisters Louise and Natalie Brown were able to give birth to perfectly healthy babies conceived naturally.
– Having analyzed the results of 3 thousand IVF procedures, scientists came to the conclusion that it is better to do the protocols in spring or summer. At this time of the year a woman’s body becomes more sensitive to gonadotropic hormones which regulate the ovaries.